Obstetric fistula is one of the most serious and tragic childbirth injuries. A hole between the birth canal and bladder and/or rectum, which is caused by prolonged, obstructed labour without access to timely, high-quality medical treatment. It leaves women leaking urine, faeces or both, and often leads to chronic medical problems, depression, social isolation and deepening poverty. There are an estimated two to 3.5 million women living with fistula with an estimated 50,000 to 100,000 new cases each year. In the Arab region, women in Yemen, Somalia and Sudan are most affected.
Yet fistula is almost entirely preventable. Its persistence is a reminder of gross inequities, a sign of global inequality and an indication that health and social systems are failing to protect the health and human rights of the poorest and most vulnerable women and girls. As the leader of the global Campaign to End Fistula, UNFPA provides strategic vision, technical guidance and support, medical supplies, training and capacity building, as well as funds for fistula prevention, treatment and social reintegration and advocacy programmes. UNFPA also strengthens sexual and reproductive health care including timely and quality emergency obstetric services to prevent obstetric fistula from occurring in the first place.
How it happens
Without emergency intervention, obstructed labour can last for days, resulting in death or severe disability. The obstruction can cut off blood supply to tissues in the woman’s pelvis. When the dead tissue falls away, she is left with a hole – a fistula, in medical terms – in the birth canal.
Tragically, there is a strong association between fistula and stillbirth, with research indicating that approximately 90 per cent of women who develop obstetric fistula end up delivering a stillborn baby.
Obstetric fistula has been virtually eliminated in industrialized countries through the availability of timely, high-quality medical treatment for prolonged and obstructed labour – namely, Caesarean section.
Obstetric fistula occurs mostly among the poorest and most marginalized women and girls, especially those living far from medical services and those for whom services are not accessible, affordable or acceptable. Childbearing in adolescent girls before the pelvis is fully developed, as well as twin pregnancy, breech position of the baby, malnutrition, small stature and generally poor health conditions are among the physiological factors contributing to obstructed labour. However, any woman may experience obstructed labour, including older women who have already had babies.
Consequences for women
Left untreated, obstetric fistula causes chronic incontinence and can lead to a range of other physical ailments, including frequent infections, kidney disease, painful sores and infertility. The physical injuries can also lead to social isolation and psychological harm: Women and girls with fistula are often unable to work, and many are abandoned by their husbands and families, and ostracized by their communities, driving them further into poverty and vulnerability. The continued occurrence of obstetric fistula is a human rights violation, reflecting the marginalization of those affected and the failure of health systems to meet their needs. Their isolation means they often go unnoticed by policymakers, and little action is taken to address or prevent their condition. As a result, women and girls suffer needlessly, often for years, with no hope in sight.
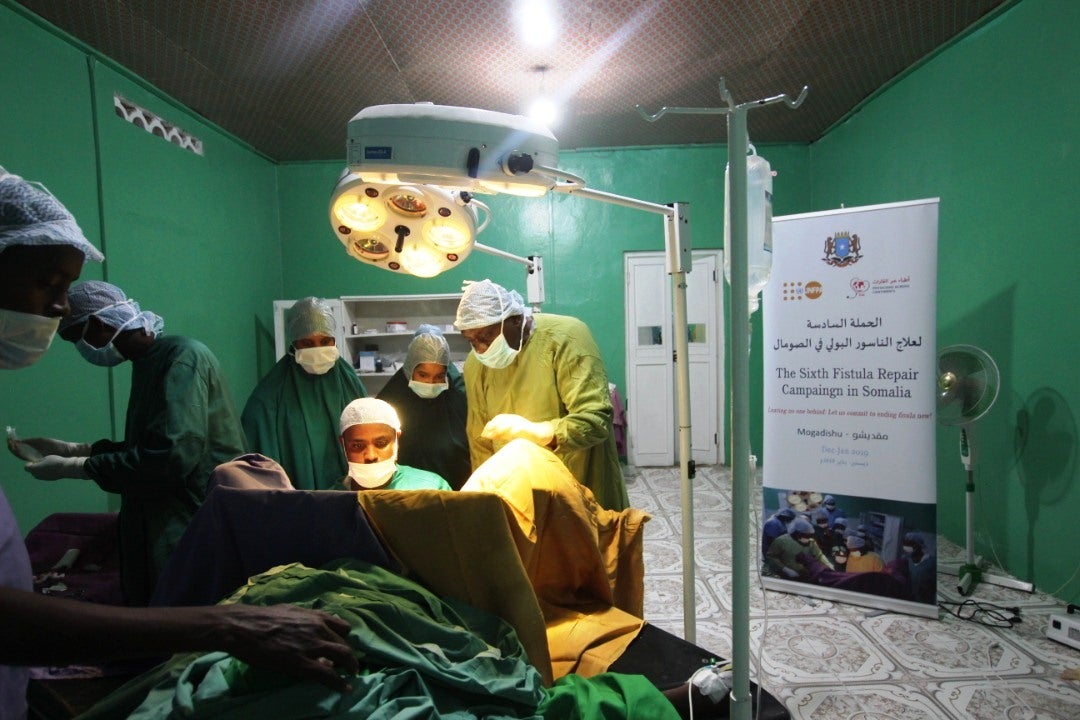
Treatment, reintegration and follow-up
Reconstructive surgery can usually repair a fistula. Unfortunately, the women and girls affected by this injury often do not know that treatment is possible, cannot afford it or cannot reach the facilities where it is available. There is also a shortage of highly trained and skilled surgeons to perform the repairs. Tragically, at the current rate of progress, many women and girls living with fistula today could die before ever being treated.
Beyond surgery, a holistic approach that addresses the psychosocial and socioeconomic needs of fistula survivors is required to ensure full recovery and healing.

Counselling and other forms of support – such as livelihood skills, literacy, job training and health education – may also be necessary to help women reintegrate into their communities, rebuild their lives, and regain their dignity and hope after surviving fistula.
Follow-up is also crucial for all women and girls who have had fistula repair surgery, helping to ensure they do not develop the injury again during subsequent births and to protect the survival and health of both mother and baby. Women and girls who have been deemed inoperable or incurable also require special and sustained attention and support.
Prevention is key
Prevention is the key to ending fistula. Fistula is an indicator of poor quality of care. Ensuring skilled birth care at all births and providing timely and high quality emergency obstetric care for all women and girls who develop complications during delivery would make this tragic condition as rare in developing countries as it is in the industrialized world.
Additionally, providing family planning to those who want it could significantly reduce maternal disability and death.

The underlying factors that contribute to women’s and girls’ marginalization – including lack of access to quality health services and education, persistent poverty, gender and socioeconomic inequality, child marriage, adolescent pregnancy, and failure to protect human rights and empower women and girls – must also be addressed.
UNFPA's response in the Arab region
UNFPA works with governments and partners to prevent obstetric fistula from occurring, as well as supporting treatment for obstetric fistula in the worst-affected countries.
In Yemen, years of conflict have decimated the health system, which heavily impacts on women’s reproductive health. UNFPA works to improve access to emergency obstetric and newborn care, trains health professionals with midwifery skills, and provides family planning services. In 2023, UNFPA supported the establishment of two fistula treatment centres at the Al Sadaqa Hospital in Aden and Al Thawra Hospital in Sana'a. The centre’s aim is to provide free surgical treatment and care to over 100 fistula patients each year.

The onset of conflict in Sudan in 2023 disrupted progress, yet UNFPA was able to support fistula treatment campaigns, fistula repairs and the training of surgeons in 2023. Fistula treatment campaigns were conducted in the Blue Nile State in November 2023, where 49 patients were surgically repaired, and three obstetricians received on-the-job training.
In Somalia, a national fistula elimination strategy has been developed with an accompanying operational plan. Routine fistula repair services have now been initiated at the National Fistula Centre in Mogadishu, and UNFPA supported more than 100 fistula repairs in 2023. More than 70 per cent of survivors received a social reintegration package after surgery. The main challenge is Somalia’s ongoing dependence on international obstetric fistula surgeons.
At the regional level UNFPA advocates for universal health coverage, which is inclusive of sexual and reproductive health services, to tackle obstetric fistula in a holistic manner. In humanitarian crises, UNFPA supports the implementation of the minimum initial service package for reproductive health, which include swift and essential services that can prevent death, disease, and disability related to unintended pregnancy, obstetric complications, sexual and other forms of gender-based violence, HIV infection, and a range of reproductive disorders. The UNFPA regional office also works to raise awareness and funds to support the obstetric fistula programmes in the region.
Updated 15 April 2024


