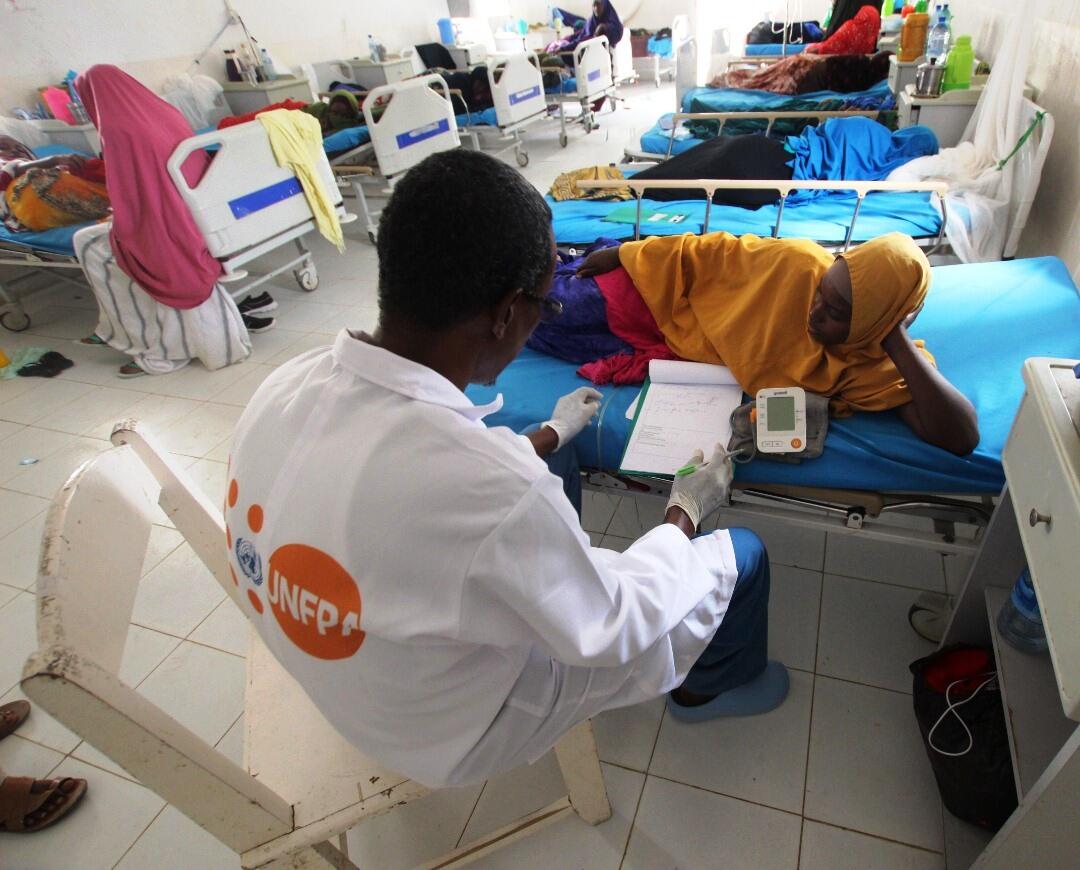
“I had no idea that my situation was redeemable,” says Ashikiro Guure Cali who recovered from obstetric fistula, after 50 years of endless suffering. She lived with one of the most demeaning medical nightmares any woman could suffer.
Ms. Cali, 70 years old, comes from Elbuur district, some 377 kilometres from Mogadishu, Somalia.. Ms. Cali, a single mother, gave birth when she was 20-years-old and sustained athe fistula injury after an obstructed labour that lasted for three days. She could no longer control the flow of urine from her body after the ordeal.
“Luckily, the baby boy survived without any complications.It was a home delivery as there was no health facility in the area,” says Cali. “I was leaking urine for the last 50 years. I have been an outcast in my own community as people didn’t want to associate with me due to the stench from the urine.” she explains with sadness.
“One day, I heard on the radio that women who have obstetric fistula have a chance to access surgical repairs at Daynile Hospital in Mogadishu. I told my son who immediately made all arrangements to take me to the hospital.”
UNFPA supports the health sector in Somalia, including public and private entities and NGOs, to run three main fistula centres in Mogadishu, Puntland and Somaliland to end obstetric fistula in Somalia by 2030.
Obstetric fistula is preventable; it can largely be avoided by preventing child marriage and adolescent pregnancy, abondaning harmful traditional practices, ensuring skilled birth care at all births and providing timely and high quality emergency obstetric care for all women and girls who develop complications during delivery.
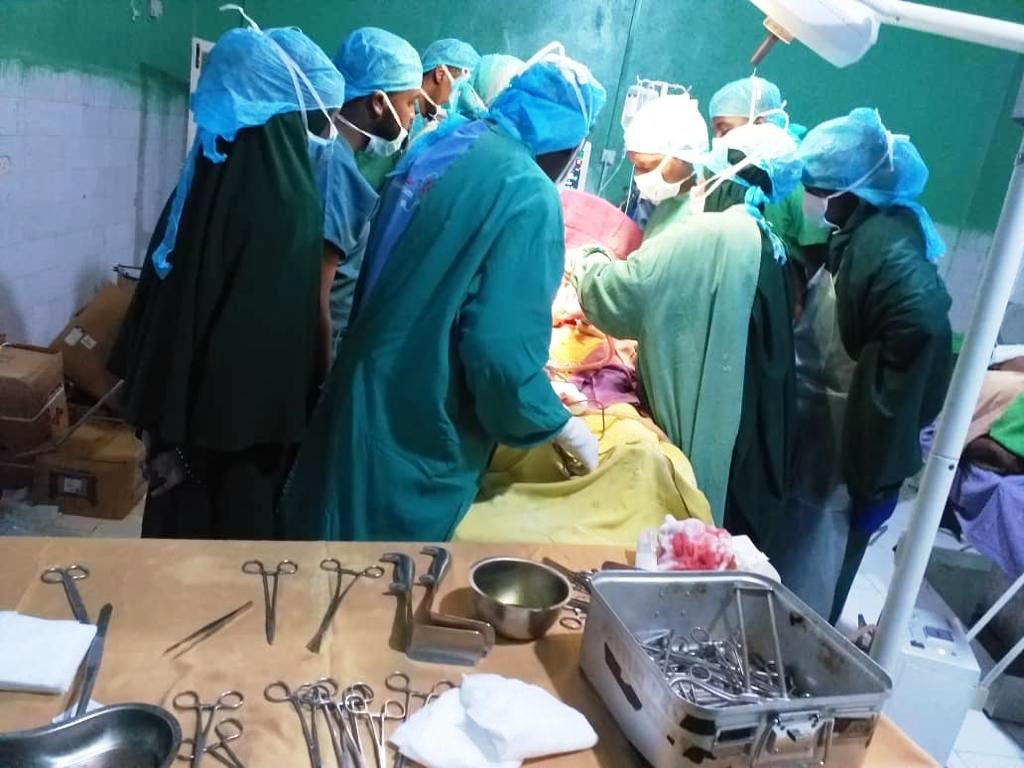
Dr. Mohamed Abdirahman, Senior Health Advisor of Physicians Across Continents (PAC) - one of the organizations that carry out fistula repair surgeries - mentioned that the same delays that cause maternal mortality are also a causal risk factor of fistula. The failure to seek timely and quality health care during obstructed labour is the main reason. This is sometimes due to social norms and cultural barriers such as the belief of traditional birth attendants and seeking the permission of the mother-in-law and husband.
A good proportion of Somalis live in rural areas. Some are nomads and do not have defined and stable settlements and move around in hard-to-reach areas. Pregnant mothers are unable to reach health facilities in good time.
Dr. Abdirahman mentioned that the quality of services delivered in the country’s health facilities are poor. “Some of the facilities might be adequately equipped, but have less motivated and overworked health care providers who do not get regular salaries. Other facilities are not able to function 24/7 due to the short in funding, supplies and staff” he said.
The Former Minister of Humanitarian and Disaster Management of the Federal Government of Somalia (FGS) and a Fistula Champion, Dr. Maryam Qasim, believes that the continuity of fistula implies a lack of access to sexual and reproductive health services and an inadequate continuum of care during pregnancy, including antenatal care (ANC), management of pregnancy complications and safe deliveries by skilled birth attendants (SBA).
According to the Somali Health and Demographic Survey 2020, only 32 percent of women giving birth in Somalia have been assisted by a skilled health provider. Dr. Qasim underscores that Somalia would eradicate fistula if access and utilization of maternal health services during pregnancy could be universal to all women of child-bearing age. “The need for tackling child marriage and girls’ education and illiteracy, and for improving the demand on skilled birth care at the grass-root level is paramount,” she says.
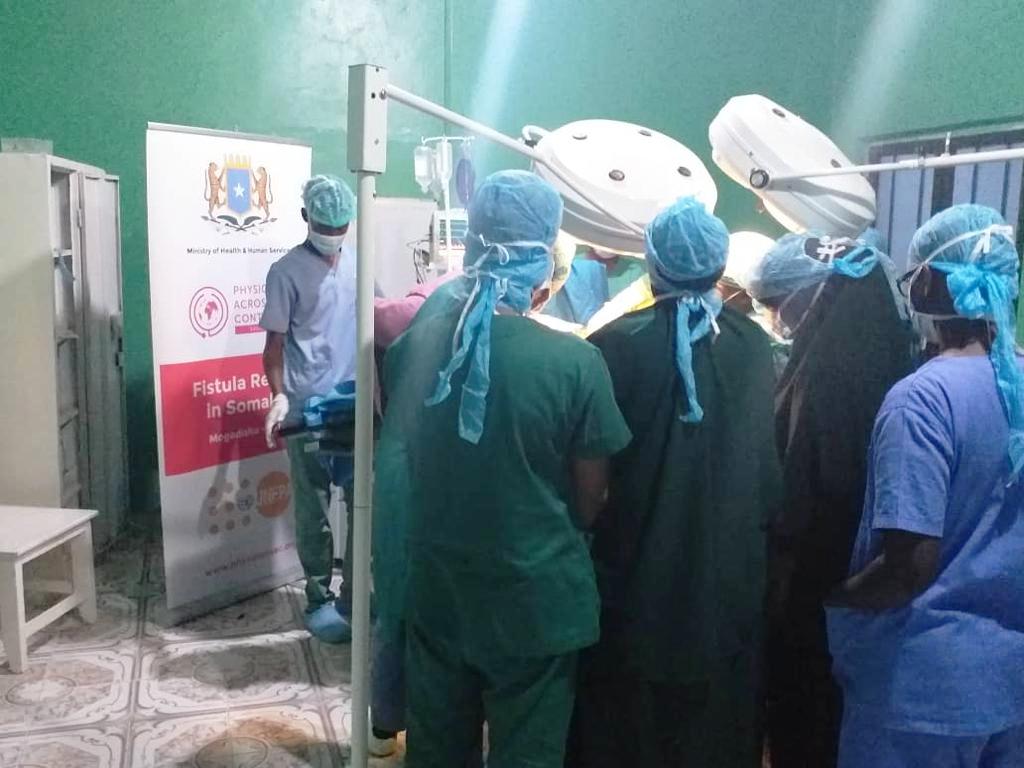
The Ministry of Health and Human Services of the Federal Government of Somalia and the Federal member states show their commitment to eradicating fistula in Somalia. The number of fistula survivors in Somalia is unknown for many reasons, but the stigma is an overpowering influence on many women who prefer to go uncounted. One in 20 women would die in the country due to pregnancy-related complications.
The COVID-19 pandemic has become a significant threat to the gains and improvement made in the access to quality midwifery and Emergency Obstetric and Newborn (EmONC ) services, not only in Somalia but around the globe. Access to repair surgeries have suffered due to lockdowns. The doctors who perform surgery come from abroad fail to have easy access to health facilities due to restrictions associated with the pandemic.
UNFPA estimates that COVID-19 could result in an additional 13 million child marriages taking place globally that otherwise would not have occurred between 2020 and 2030. All of these issues could affect the incidence of obstetric fistula.
To date, UNFPA, as the leader of the global Campaign to End Fistula , has directly supported more than 113,000 surgical repairs for women and girls, and partner agencies have supported thousands more. These treatments help to restore survivors' health and hope, empowering them to reclaim their lives and dignity.