Around 800 women die each day from preventable causes related to pregnancy and childbirth. This is about one woman every two minutes. For every woman who dies, between 20 and 30 will experience injuries, infections or disabilities. Most of these deaths and injuries are entirely preventable. A majority of them die from severe bleeding, sepsis, eclampsia, obstructed labour and the consequences of unsafe abortions – all causes for which there are highly effective interventions. And the tragedy does not stop there, when mothers die, their families are much more vulnerable, and their infants are less likely to reach their second birthday.
Making motherhood safer is a human rights imperative, and it is at the core of UNFPA’s mandate. UNFPA works around the world with governments, health experts and civil society to train health workers, improve the availability of essential medicines and reproductive health services, strengthen health systems, and promote international maternal health standards.
Commendable yet uneven progress
The Arab region achieved a 45% reduction in its maternal mortality ratio between the year 2000 and 2020, with a decrease from 260 deaths per 100,000 live births in 2000 to 145 in 2020. Yet huge discrepancies exist between countries, including those that face protracted humanitarian crises.
In most Arab countries, maternal deaths have decreased as women gained access to family planning, skilled birth attendance and emergency obstetric care. While most Arab countries have already met the Sustainable Development Goals’ target of achieving below 70 maternal deaths per 100,000 live births by 2030, progress stagnated across the region from 2015-2020. Furthermore, the maternal mortality rate remains above 200 deaths per 100,000 live births in Djibouti, Somalia, Sudan and Yemen as these countries struggle with protracted crises.
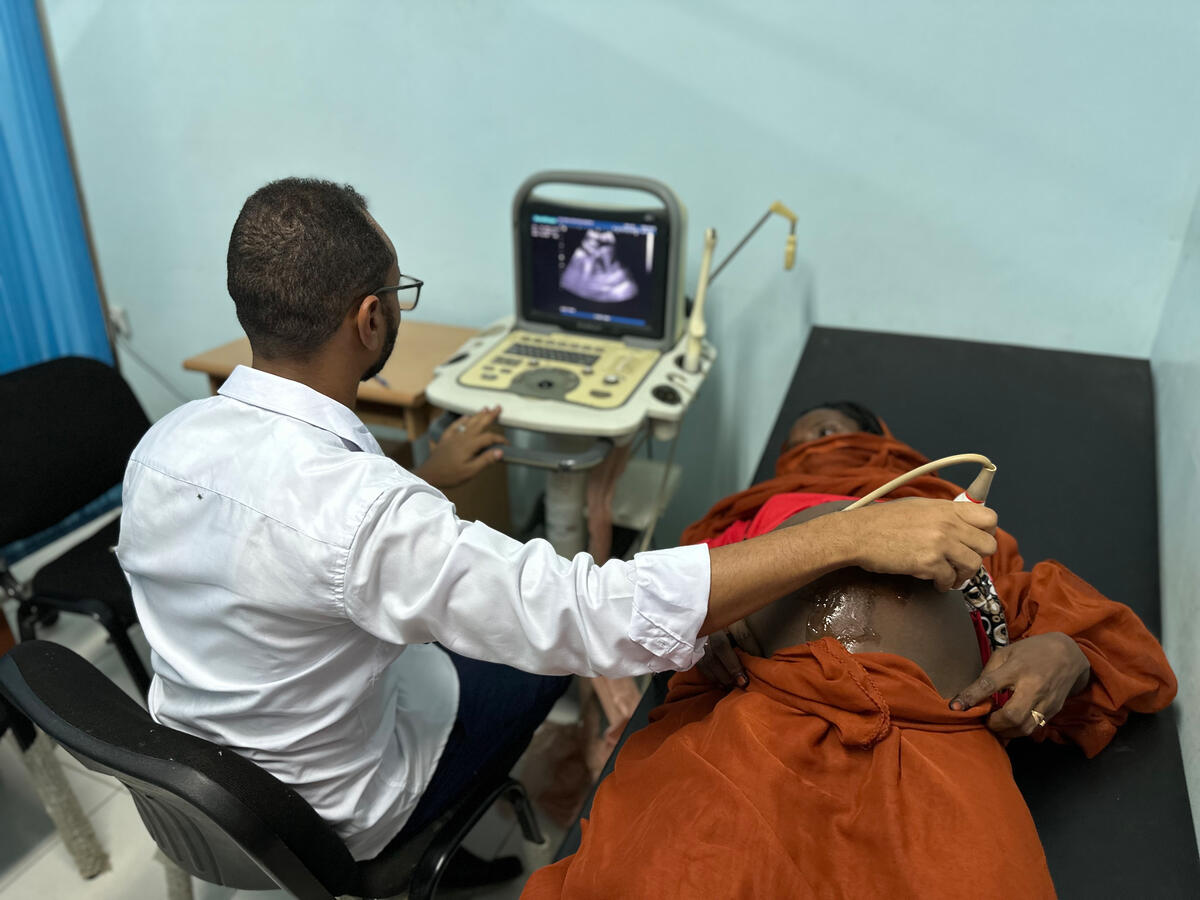
The best way to achieve the Sustainable Development Goals maternal mortality reduction target is to ensure all women have access to contraception to avoid unintended pregnancies, to provide all pregnant women with skilled and respectful care in safe environments during delivery, and to ensure women with complications have timely access to quality emergency obstetric care.
Antenatal care
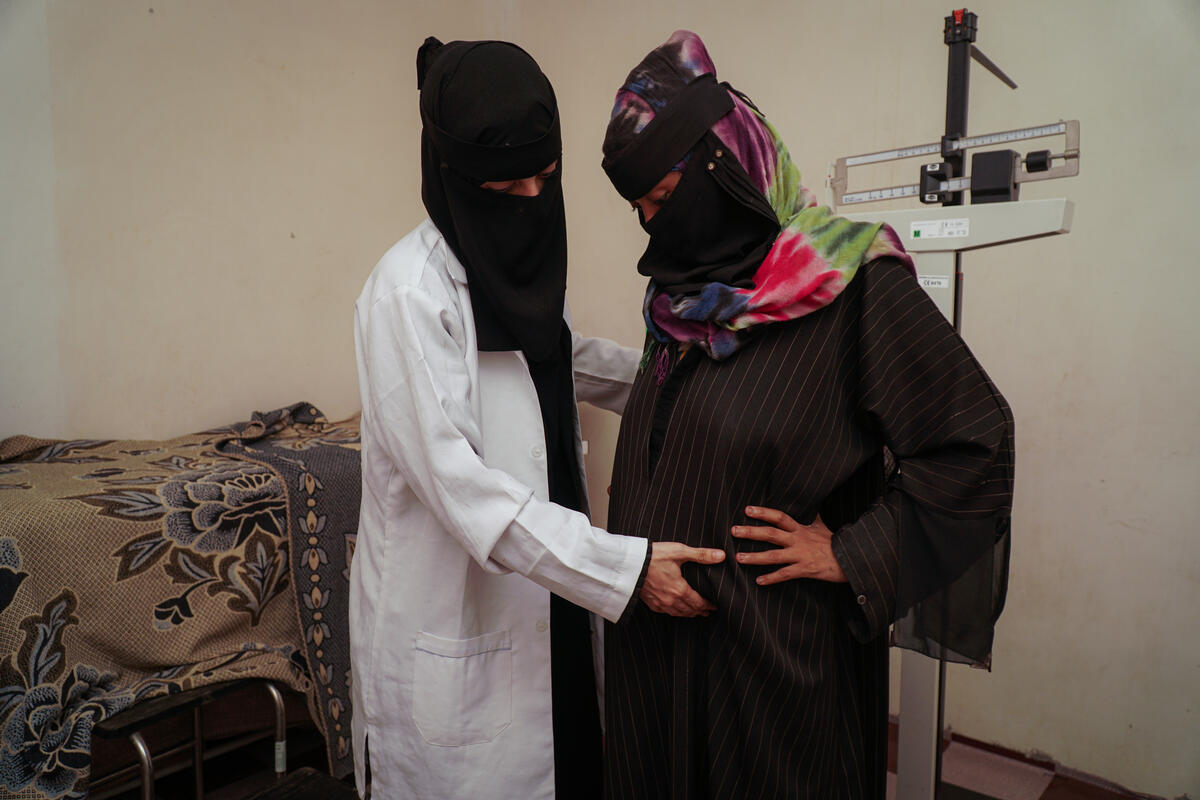
Antenatal care is care that is provided by health professionals during pregnancy. It is an important part of basic maternal health care. The World Health Organization (WHO) recommends expectant mothers receive at least eight antenatal care visits, in which a health worker can check for signs of ill health – such as being underweight, anaemia, hypertension, or infection – and monitor the health of the fetus. During these visits, women are counselled on nutrition and hygiene to improve their health prior to, and following, delivery. UNFPA and WHO strongly recommend they develop a birth preparedness and complication readiness plan, an essential component of antenatal care, which lays out how to receive care and what to do in case of an emergency.
Because these visits may be a woman’s first interaction with the health system, they are an important opportunity to assess their overall health, and to speak with them about their sexual and reproductive health and rights. They can be advised on choosing a modern contraceptive method appropriate for them and learn about the health benefits of spacing births and how to plan their families. They are also counselled on newborn care, post-delivery family planning and the importance of birth registration.
Nonetheless, the great majority of obstetric complications are unpredictable, arising with little or no warning. While antenatal visits may not prevent most complications, some can be identified and addressed in a timely manner, and women who receive antenatal care are more likely to deliver with the help of a skilled birth attendant who can recognize and address these issues.
Skilled birth attendance
Skilled attendance at birth, with emergency backup, is considered the most critical intervention for ensuring safe motherhood. Skilled birth attendants are health workers, such as doctors, nurses or midwives, who have the skills to manage normal deliveries and recognize the onset of complications. They perform essential interventions, start treatment, manage some basic complications and supervise the referral of other complications to comprehensive emergency care. Skilled attendance is also vital for protecting the health of newborns, as the majority of perinatal deaths occur during delivery or in the 48 hours afterward.

Skilled attendance requires an enabling environment, such as a clean delivery area with the necessary supplies and equipment. And skilled birth attendants must provide respectful care that takes into account the dignity of the pregnant woman. Unfortunately, many countries have severe shortages of trained health providers with midwifery skills.
Emergency obstetric care
Emergency obstetric care is critical to reducing maternal mortality. All five of the major direct causes of maternal death – haemorrhage, sepsis, unsafe abortion, hypertensive disorders and obstructed labour – can be treated at a well-staffed, well-equipped health facility. In such settings, most newborns with asphyxia or infection can also be saved.
In case of complications, all women and newborns should have rapid access to well-functioning emergency obstetric facilities that meet good quality-of-care standards. And in the long term, all births should take place in appropriate facilities, as is the case in all countries that have managed to significantly reduce their maternal mortality.
Postnatal care
Postnatal care – provided within the first 24 hours of delivery, on the third day afterward, then in the second and sixth weeks – is also critically important. Bleeding, sepsis and hypertensive disorders can all occur after a woman leaves the health facility. Furthermore, postnatal checks provide an opportunity for health workers to check a mother’s mental health and wellbeing. Newborns are also extremely vulnerable in the immediate aftermath of birth.
UNFPA, WHO and UNICEF strongly recommend follow-up visits by a health worker to assess both mother and child in the postnatal period.
UNFPA at work
Making motherhood safer is a top priority for UNFPA. UNFPA works at all levels to promote universal access to sexual and reproductive health care and rights, including by promoting international maternal health standards and providing guidance and support to health systems, including advocacy related to financing the ICPD agenda.

In the Arab region, UNFPA-supported programmes emphasise capacity development in maternal care and midwifery, especially in strengthening of human resources and emergency obstetric and newborn care.
UNFPA helps to train midwives, supports emergency obstetric and newborn care facilities and networks, and provides essential drugs and family planning services. UNFPA also supports the implementation of maternal death and perinatal response systems, which help officials understand how many women are dying, why, and how to respond, ensuring the integration of evidence generated from robust studies into policies and systems development.
Recognizing that maternal mortality and morbidity remains especially high in poor, fragile and crisis affected countries, where more than a third of global maternal deaths occur, UNFPA in the Arab region seeks to make pregnancy and childbirth as safe as possible in these settings.
A key contribution to improving the situation of maternal health in the region is to ensure the implementation of the Minimum Initial service Package of sexual and reproductive health in crisis affected countries and the integrated approach to addressing obstetric fistula in the region in the countries where it is most reported such as Djibouti, Somalia, Sudan and Yemen.
UNFPA is also strengthening its regional focus to “finance the ICPD agenda” through efforts to influence health financing, universal health coverage, and private sector engagement. Data shows that investments in family planning and maternal health have a high return on investment. In fact, data collected from 12 countries in the Arab region demonstrates that for every $1 spent in ending the unmet need for family planning and preventable maternal deaths in 12 countries in the Arab region, $5 in returns can be expected.
Updated 30 July 2024


